Table of Contents
Introduction
Harlequin fetus, medically known as Harlequin ichthyosis, is one of the rarest and most severe congenital skin disorders observed at birth. Characterized by thick, plate-like scales covering the entire body, this condition represents the most extreme form of inherited ichthyosis.
Historically, the prognosis for babies born with this disorder was extremely poor. However, with modern neonatal intensive care, genetic diagnosis, and advanced dermatological treatments, survival rates have significantly improved.
This comprehensive guide explains everything about harlequin fetus — including its causes, genetic basis, clinical presentation, diagnosis, treatment options, long-term survival, and current medical advancements.
Key Medical Takeaways
- Harlequin fetus is caused by ABCA12 gene mutation.
- It follows autosomal recessive inheritance.
- Immediate NICU care improves survival chances.
- Oral retinoids significantly enhance outcomes.
- Long-term care is essential for survivors.
What Is a Harlequin Fetus?
Harlequin fetus refers to a newborn affected by Harlequin ichthyosis, a severe genetic disorder that disrupts the development of the outermost layer of skin (epidermis). Babies born with this condition present with:
- Thick, armor-like plates of hardened skin
- Deep fissures separating the plates
- Severe facial deformities due to tight skin
- Restricted movement of limbs
- Compromised breathing
The condition is present at birth and requires immediate medical intervention.
Why Is It Called “Harlequin”?
The term “harlequin” originates from the distinctive diamond-shaped pattern formed by the thick, hardened skin plates seen in newborns with Harlequin ichthyosis. These large, polygonal plates are separated by deep fissures, creating a geometric appearance that historically reminded physicians of the costume worn by the Harlequin, a character from traditional Italian theater known as Commedia dell’arte.
In classic theatrical performances, the Harlequin character wore a colorful outfit made up of diamond-shaped patches stitched together in a repeating pattern. When early medical observers encountered infants born with this rare and dramatic skin presentation, they used the term “harlequin fetus” because the hardened, plate-like scales resembled that patterned costume.
Historical Context of the Term
Medical terminology in earlier centuries often relied on visual analogies to describe rare or unusual conditions. Because Harlequin ichthyosis presents with:
- Large, thickened keratin plates
- Deep red fissures dividing the plates
- A symmetrical, geometric skin pattern
the theatrical comparison became widely adopted in early case reports and dermatological literature.
Over time, the term “harlequin fetus” became commonly used in textbooks, medical journals, and case documentation to describe newborns affected at birth.
Causes and Genetic Basis
The ABCA12 Gene Mutation
Harlequin ichthyosis is caused by mutations in the ABCA12 gene, which plays a critical role in transporting lipids to the outer layer of the skin.
Lipids are essential for:
- Maintaining skin barrier integrity
- Preventing water loss
- Protecting against infections
- Regulating body temperature
When the ABCA12 gene is defective, lipid transport fails. This leads to abnormal keratinization and thickened skin plates.
Inheritance Pattern
Harlequin fetus follows an autosomal recessive inheritance pattern.
What This Means:
If both parents are carriers of the mutated gene:
| Outcome | Probability |
| Affected child | 25% |
| Carrier child (no symptoms) | 50% |
| Unaffected, non-carrier | 25% |
Carriers typically show no symptoms but can pass the gene to their offspring.
Risk Factors
While the condition is rare, certain factors increase risk:
- Parents who are both carriers
- Family history of ichthyosis
- Consanguineous marriage (marriage between close relatives)
- Previous child affected with harlequin ichthyosis
Clinical Features and Symptoms
Physical Appearance at Birth
Babies with harlequin fetus typically show:
| Symptom | Description |
| Thick hyperkeratotic plates | Large, hard skin scales covering the body |
| Deep fissures | Painful cracks between skin plates |
| Ectropion | Eyelids turned outward |
| Eclabium | Lips pulled outward |
| Flattened nose | Due to tight skin |
| Small or poorly formed ears | Restricted development |
| Limb stiffness | Limited movement |
Systemic Complications
The skin is a vital organ for fluid regulation and protection. When severely compromised, the following complications may occur:
- Respiratory distress
- Severe dehydration
- Electrolyte imbalance
- Temperature instability
- Increased infection risk
- Feeding difficulties
These complications require immediate NICU management.
Prenatal Diagnosis
Early detection is possible, especially in high-risk pregnancies.
Diagnostic Methods
| Method | Purpose |
| Ultrasound | May detect abnormal facial features or skin thickening |
| Amniocentesis | Genetic testing for ABCA12 mutation |
| Chorionic Villus Sampling (CVS) | Early genetic diagnosis |
| Family history screening | Risk assessment |
Early diagnosis allows parents to prepare for specialized neonatal care.
Management and Treatment
There is currently no cure for harlequin ichthyosis. Treatment focuses on supportive care and complication prevention.
Immediate Neonatal Care
After birth, babies are typically admitted to a Neonatal Intensive Care Unit (NICU).
Key interventions include:
- Humidified incubator care
- Temperature control
- Intravenous fluids
- Electrolyte monitoring
- Broad-spectrum antibiotics
- Pain management
Role of Retinoids
Oral retinoids such as acitretin or etretinate have shown improved survival rates.
Benefits of Retinoid Therapy:
- Accelerates shedding of thick skin
- Reduces plaque formation
- Improves mobility
- Enhances skin barrier formation
Early initiation significantly improves outcomes.
Supportive Dermatological Care
Long-term management includes:
- Frequent application of emollients
- Petroleum-based moisturizers
- Gentle wound care
- Eye lubrication for ectropion
- Physical therapy for joint movement
Survival Rates: Then vs Now
Historically, most infants with harlequin fetus died within days due to complications.
Survival Comparison
| Era | Survival Outcome |
| Before 1980 | Majority died within first week |
| 1980–2000 | Improved survival with retinoids |
| Modern era | Up to 50% survive infancy |
| With advanced care | Some survive into adulthood |
Medical advancements have dramatically changed the prognosis.
Long-Term Outlook
Children who survive infancy typically experience:
- Persistent skin scaling
- Chronic dryness
- Increased infection risk
- Delayed growth in some cases
- Joint stiffness
However, cognitive development is generally normal.
Many survivors attend school, live active lives, and require ongoing dermatological care.
Comparison with Other Ichthyosis Types
| Condition | Severity | Onset | Life Expectancy |
| Harlequin ichthyosis | Most severe | At birth | Variable |
| Lamellar ichthyosis | Moderate | Birth | Near normal |
| Ichthyosis vulgaris | Mild | Childhood | Normal |
Harlequin ichthyosis remains the most life-threatening form.
Global Incidence
Harlequin fetus is extremely rare.
Estimated Frequency
| Region | Estimated Incidence |
| North America | 1 in 300,000–500,000 births |
| Europe | Similar estimates |
| Asia | Underreported but comparable |
| Global | Less than 200 cases reported historically |
Because it is rare, exact data varies.
Cost of Treatment and Care
Managing harlequin ichthyosis involves long-term medical care.
Estimated Medical Cost Differences
| Treatment Phase | Estimated Cost Range (USD) |
| Initial NICU stay | $50,000 – $200,000 |
| Genetic testing | $500 – $2,000 |
| Annual dermatological care | $5,000 – $15,000 |
| Lifetime care (approx.) | Varies widely |
Costs depend heavily on country and healthcare system.
Harlequin Ichthyosis Care Cost Breakdown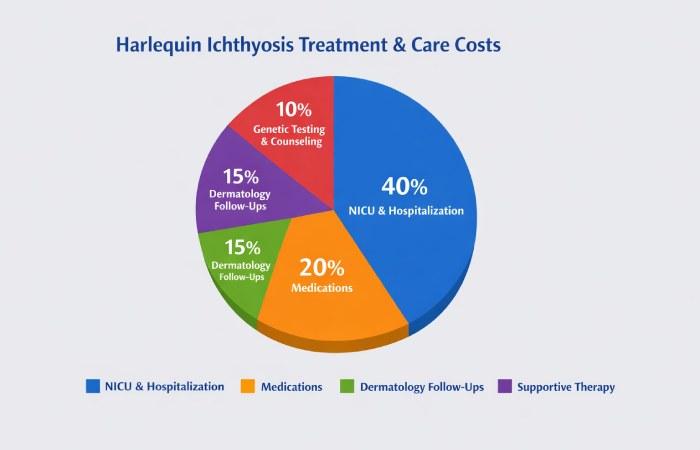
Genetic Counseling and Prevention
Couples with known carrier status should consider:
- Preconception genetic counseling
- Prenatal genetic screening
- IVF with genetic testing (in some regions)
Counseling helps families make informed reproductive decisions.
Emotional and Psychological Impact
Parents may experience:
- Shock at diagnosis
- Grief and anxiety
- Long-term caregiving stress
Psychological support is strongly recommended.
Frequently Asked Questions
Is harlequin fetus always fatal?
No. While historically fatal, many infants now survive with advanced medical care.
Can it be detected before birth?
Yes. Genetic testing can identify the ABCA12 mutation during pregnancy.
Is it contagious?
No. It is a genetic disorder and cannot spread.
Can survivors live normal lives?
Many survivors live into adolescence and adulthood with ongoing care.
Conclusion
Harlequin fetus, or Harlequin ichthyosis, remains one of the most severe congenital skin disorders known in medicine. However, advancements in neonatal care, dermatological therapy, and genetic testing have transformed what was once considered universally fatal into a condition where survival is increasingly possible.
While challenges remain, early diagnosis, intensive treatment, and long-term care have improved both life expectancy and quality of life.
Continued research, awareness, and access to medical support will further improve outcomes for families affected by this rare genetic condition.
